
Managing Nutrition during Cancer and Treatment
Good Nutrition and Cancer Treatment
Good nutrition is very important during cancer treatment. Eating well during treatment can improve the effectiveness of your cancer treatments, which can lead to better outcomes.
Malnutrition, a condition that occurs when the body lacks nutrients, is a common problem in cancer patients. Malnutrition can occur in people of any weight status (underweight, healthy weight, and overweight). Malnutrition can lead to poor outcomes and treatment delays. To help protect against malnutrition, eat at least three meals each day, plus snacks. Be sure to include all food groups. Include protein foods at each meal. Examples of protein foods are chicken, turkey, fish, eggs, Greek yogurt, cottage cheese, beans/lentils, nuts, seeds, tofu, and milk. In addition, you will need to drink lots of fluid each day (at least 80-100 oz. per day) in order to stay hydrated. Water is usually the best fluid to drink.
Unintentional weight loss during cancer treatment can also lead to worse outcomes for patients with cancer. Both malnutrition and weight loss can make it harder for the body to rebuild healthy cells between chemotherapy cycles. This can lead to delays in treatment schedules and prevent successful treatment outcomes. Weigh yourself at least one time each week to make sure you aren't losing weight. Even a small amount of weight loss (such as 10-20 pounds or more for a person who normally weighs 200 pounds) during treatment may lead to worse outcomes.
The body uses calories and protein for fuel to support healthy organs, muscle repair, and daily activity. Your body needs more calories and proteins during most types of cancer and treatments. The extra calories and protein are used to heal tissues and fight infections during chemotherapy or radiation therapy, or after surgery. For this reason, most people going through cancer treatment have to eat more than they are used to eating. Otherwise, they can become malnourished and lose weight.
If you appetite is good and you are currently maintaining your weight, it's a good idea to eat a balanced diet and include a variety of healthy foods. Try to include foods from this list at each meal. It is fine to have other foods as well.
Foods to Enjoy
- Protein Foods: Plant proteins like beans, lentils, and soy, as well as lean animal proteins like chicken, turkey, fish, and seafood, and eggs.
- Fruits and Vegetables: Choose a variety of colorful fruits and vegetables.
- Low Fat Dairy and Dairy Alternatives (cow, soy, almond, rice etc.): milk, cheese, Greek yogurt, cottage cheese, and kefir. Dairy foods are often good protein sources.
- Whole Grains and Starchy Vegetables: oats, quinoa, barley, brown rice, popcorn, corn, potatoes, peas, winter squash, and 100% whole grain bread, pasta, cereal, and crackers.
- Nutritious Fats: olive oil, canola oil, nut butters (such as peanut butter or almond butter), avocado, nuts, and seeds.
- Beverages: water, tea, coffee (especially decaf), milk, and diluted juice.
During treatment, you may find that your appetite is not great or that you have side effects that make it hard to eat healthfully. When you are not able to maintain your weight with foods that are traditionally considered healthy, it is fine to choose other foods that appeal to you. However, be sure to still include enough fluids, protein, and calories to prevent malnutrition.
Think of eating as part of your treatment. Whether or not you are hungry, you need to eat regularly in order to have enough fuel in your body to fight cancer and preserve your muscle. If you do not eat regularly, you will likely lose weight and may become malnourished, meaning your treatment may not work as well and it will be harder to heal following surgery and treatments.
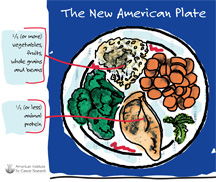
A well-balanced diet should include every food group, including lots of plant foods. This type of diet contains vitamins, minerals, and phytochemicals needed to help your body fight cancer. The New American Plate (pictured below) was developed by the American Institute for Cancer Research. This picture shows what a healthy meal can look like. When planning your meals, aim to cover most of each plate (at least 2/3) with plant foods like fruits, vegetables, beans, and whole grains. The rest of the plate (1/3) can include animal foods like chicken, fish, eggs, cheese, and yogurt.
For information on modified diets or managing nutrition related side effects click on the links below:
For more information on nutrition recommendations during cancer treatment and for cancer prevention, click on the links below:
- National Cancer Institute: Eating Hints Booklet
- The American Cancer Society: Nutrition for People with Cancer
Key points:
- Eat at least 3-6 times per day, choosing from all food groups. Be sure to include protein foods with each meal.
- Drink at least 80-100 oz of fluid per day, mostly from water
- Weight yourself at least once per week to see if you are losing weight. If you are losing weight, eat more frequently and talk to your doctor, nurse, or dietitian about ways to eat more.
- If you aren't able to tolerate healthy foods, eat whatever you can tolerate. You still need to eat enough to maintain your weight and muscle mass, as well as staying well hydrated.
Due to variation in specific illness and treatment plans, eating practices of individuals diagnosed with cancer should be assessed throughout the continuum of care. Request an appointment with a registered dietitian at your treatment facility for a comprehensive nutrition assessment and tailored nutrition therapy plan to reflect your personal treatment goals.
To make an appointment with a dietitian at a Cleveland Clinic Cancer Center call:
- Main Campus (Taussig) 216-444-6833
- Hillcrest 440-312-4700 or 440-312-5560
- Fairview Moll 216-476-7606
- Sandusky 419-626-9090
- Mansfield 419-756-2122
- Wooster 330-287-4500
- Akron 330-344-2219
For patients getting cancer care at a Cleveland Clinic location:
- All nutrition visits are free of charge.
- Appointments can be scheduled during infusion treatment.
- Can schedule one-on-one in-person, virtual or phone appointments*.
*Virtual visits cannot be provided to patients in AK, CA, KS and NJ.
Clinical Trials
Search Cancer Clinical Trials
Carefully controlled studies to research the safety and benefits of new drugs and therapies.
SearchPeer Support
4th Angel Mentoring Program
Connect with a 4th Angel Mentor and speak to someone who understands.
4thangel.ccf.org
